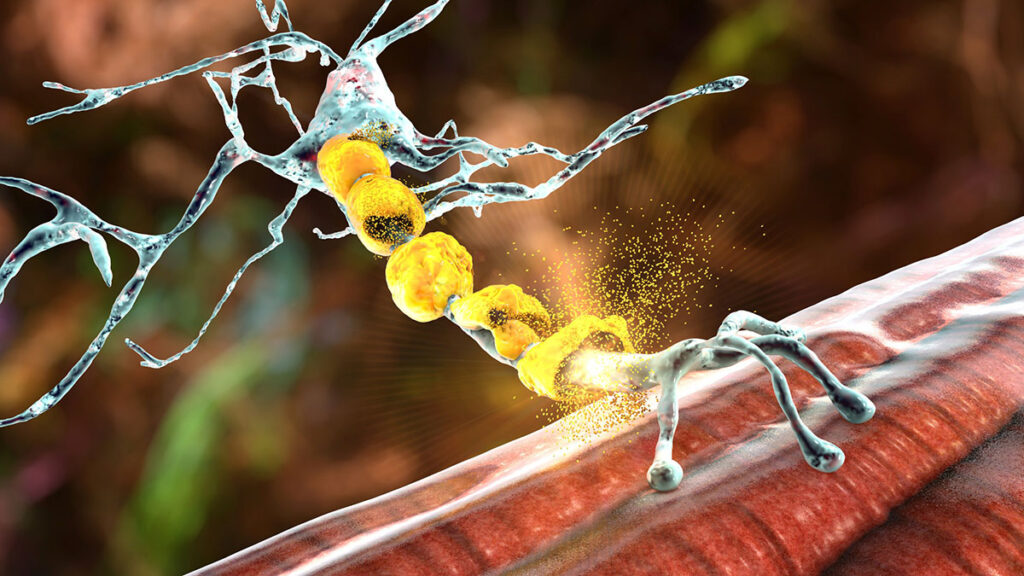
What is Motor Neurone Disease (MND)?
The term motor neuron disease (MND) covers several neurological conditions with a destructive effect on the motor neurons. The motor neurone cells play a vital role in controlling many activities, such as breathing, speaking, swallowing, and walking. Therefore, their impaired function leads to physical disability that requires extensive medical care.
This uncommon condition prevents the transmission of signals between the motor neurones and the muscles, which causes the muscles to shrink in size and become weaker (muscle wasting or atrophy). Motor neurone disease may lead to spontaneous muscle spasms and twitches visible below the skin’s surface.
Furthermore, the disrupted transmission of signals between the upper and lower motor neurons causes overactive reflexes and muscle stiffness. These irregularities in the brain and nervous system function lead to slower and more difficult voluntary movements. As MND progresses, the individual may find it hard to walk, swallow, speak, and control other types of movement.
Types of MND
Motor neurone diseases are classified according to the area they affect (upper motor neurons, lower motor neurons, or both) and whether they run in the family (genetic or sporadic). The Motor Neurone Disease Association recognises the following types of MND:
- Classical motor neurone disease – also called amyotrophic lateral sclerosis or ALS, attacks both the lower and upper motor neurons, causing drastic loss of muscle control and paralysis
- Progressive bulbar palsy (PBP) – affects the lower motor neurones linked to the brain stem and impairs the control over several functions, including speech, chewing, and swallowing
- Primary lateral sclerosis (PLS) – attacks the upper motor neurones and causes difficulty controlling the movement in the face, arms, and legs
- Progressive muscular atrophy (PMA) – a rare disease prevalent in men that slowly and progressively damages the lower motor neurones, usually diagnosed at a younger age compared to other MNDs
- Spinal muscular atrophy (SMA) – a genetic condition that attacks lower motor neurons and frequently causes infant mortality
- Kennedy’s disease – X-linked recessive disorder present in male patients, caused by gene mutations related to the androgen receptor
What Are the Early Symptoms of MND?
Many people’s early symptoms of MND are mild and generally painless or not exclusive to this disease. Therefore, patients may often get misdiagnosed with other conditions, such as stroke, multiple sclerosis, throat blockage, or respiratory disorders.
In the early stages, individuals with MDS usually experience the following symptoms:

- Muscle weakness in the limbs (a weakened grip that makes it hard to pick up or hold objects, shoulder weakness that makes it difficult to lift the arm, hip or ankle weakness that causes tripping)
- Dysphagia (difficulty swallowing)
- Dysarthria (slurred speech)
- Shortness of breath and breathing difficulties
Advanced Symptoms of MND
As the disease progresses, it will affect more body parts and their respective functions. This may also cause an increased risk of infections and related complications. In the advanced stage, MND is characterised with:
- More intense weakness and stiffness in the limbs, joint aches and movement difficulties
- Speech and swallowing difficulties with possible choking episodes
- Excessive saliva production that leads to drooling
- Uncontrollable yawning without tiredness, causing jaw pain
- Frequent changes in mood and emotional lability (for example, sudden uncontrollable crying or laughter)
- Increased breathing difficulties that become worse during the night (may require non-invasive assisted ventilation to improve sleep quality)
Final-stage Symptoms
At the final stage of MND, individuals may experience significant shortness of breath and body paralysis that makes them unable to cope with daily activities independently. More medications and invasive breathing support will be necessary to sustain the person’s body functions. Palliative and hospice care are vital in bringing relief to these patients and providing them with emotional support in their final moments.
How is Motor Neurone Disease Diagnosed?
If you are experiencing one of the previously mentioned symptoms, you should consult a specialist and undergo a neurological examination. Motor neurone disease isn’t diagnosed through a single test. Your neurologist might need several tests to rule out other potential causes for these symptoms. The examination may include the following:
- an MRI scan (magnetic resonance imaging) – involving a thorough assessment of the activity in your brain and spinal cord
- electromyography (EMG) – measuring electrical activity in the muscles and muscle responses to nerve stimulation
- lumbar puncture – testing a sample of spinal fluid to rule out a possible infection
- muscle biopsy – analysing a part of the muscle tissue to exclude other muscle diseases
- genetic testing – identifying possible gene mutations that might be the cause of developing MND
Motor neurone disease is typically diagnosed in adults and at an advanced stage of the condition. A delay in the diagnosis may occur for many reasons. Early symptoms may appear too mild or be mistakenly linked to other conditions, so the patient might not initially consult a neurologist.
Getting diagnosed with motor neurone disease is an overwhelming and life-changing event for the individual and their whole family. After the diagnosis, your doctor should connect you to healthcare professionals specialising in caring for patients with MND. Access to quality complex care at home can alleviate the physical and emotional struggles of living with motor neurone disease.
How Common is Motor Neurone Disease?
MND is a relatively rare condition that statistically affects 2 in 100 000 people annually and 5-7 in 100 000 overall. Therefore, most general practitioners have little experience with this condition, and individuals affected by it should receive support from a specialist team. Motor neurone disease is most likely to occur in male adults.
What Causes MND?
After numerous clinical trials worldwide, experts still cannot identify the cause of MND. The disease appears unrelated to race, dietary habits, or lifestyle. Furthermore, it isn’t infectious or linked to another disorder.
Age is an important factor in developing motor neurone disease. Early onset MND symptoms usually occur after age 40, whereas people between 50 and 70 constitute a large part of all patients with this condition.
Is Motor Neurone Disease Hereditary?
Family history can be a risk factor for getting diagnosed with MND at some point in your life. Experts in research trials have managed to isolate several gene mutations linked to this condition. However, genetics is rarely the cause of motor neurone disease. Hereditary cases comprise only five to 10 per cent of all registered MND cases. In the vast majority of patients, motor neuron disease develops sporadically.
Motor Neurone Disease Treatment
There is still no definite cure for motor neurone disease. However, various supportive treatment programs can significantly benefit individuals with this condition. Dedicated, multidisciplinary care from a specialist team of clinicians and support workers is essential for improving the quality of life for people with MND.
Treating motor neurone disease symptoms is possible in the following ways:
- Physical and occupational therapy – an occupational therapist can outline an exercise plan for slowing down muscle weakness and atrophy, preventing joint immobility, improving posture, reducing muscle cramps and stiffness, and increasing circulation
- Speech and language therapist arrangement and additional therapy for swallowing difficulties
- Assistive devices for improving the individual’s independence and quality of life, such as wheelchairs, speech synthesisers, braces, and orthotics
- A nutritious and balanced dietary plan for preventing drastic weight loss and maintaining strength (as chewing and swallowing become increasingly difficult, the person may need a feeding tube)
- Non-invasive ventilation to prevent breathlessness at night due to weakness in the throat, neck, and chest muscles
- Psychological support for mental health issues (anxiety, depression) that the person may experience after the diagnosis
Motor Neurone Disease Life Expectancy
The prognosis for individuals with motor neurone disease depends on several factors, including the type of MND and the age at which early onset symptoms begin. Some types of motor neurone disease, such as Kennedy’s disease and primary lateral sclerosis, usually progress slowly and may not be fatal. On the other hand, spinal muscular atrophy and amyotrophic lateral sclerosis cause a shortened life expectancy. However, with the constant medical progress, even individuals with ALS can live ten or more years after the diagnosis.
Motor Neurone Disease Final Stages
Different patients may experience different symptoms in the final stages of MND. In this phase, the affected individual may experience marked weight loss, dysphagia, respiratory failure, recurrent infection, and decline in mental abilities (some may develop frontotemporal dementia). Eventually, the breathing muscles stop working, and the patient falls into a deep sleep, resulting in a peaceful death.
With adequate complex care from dedicated support workers, individuals with this neurological disease can spend their final days fulfilled and dignified. Palliative care at home allows the person to stay near their loved ones while they receive medical assistance.
How Leaf Complex Care Supports People With MND?
At Leaf Complex Care, providing comfort and fulfilment for people with complex needs is imperative. For our trained support workers, assisting individuals with MND is not only a career but a noble mission. Our support services focus on alleviating the symptoms of MND and helping the service user with everyday tasks so that they can live as independently as possible. Practitioners in palliative care enable individuals in the end-of-life stages of MND to achieve their final goals and provide emotional support to their families.
We currently offer support services in Bristol, Slough, Somerset and the Midlands. If you have a loved one with this condition, get in touch with us via phone or email, and we will outline a tailored care plan that prioritises their specific needs.